How to practice gratitude without toxic positivity — complete with research, techniques, and free resources
Why This Isn’t A “Just Be Grateful” Post
We’ve all heard it. Someone hears about your rheumatoid arthritis and tells you to be grateful.
“At least it’s not cancer.”
“Be grateful you can still walk.”
“Think positive!”
“Others have it worse.”
These comments, while perhaps meaning well, often make people feel worse, not better. They can feel dismissive of very real pain, grief, and anger. They imply that suffering from a chronic illness isn’t valid because someone, somewhere had it “worse.”
That’s not gratitude — that’s toxic positivity. And it’s harmful.
However, I’ve learned that there’s a way to practice gratitude that doesn’t dismiss your pain, doesn’t minimize your suffering, and doesn’t require you to pretend everything is fine.
Real gratitude practice, the kind backed by research, allows you to hold two truths simultaneously.
“I am suffering AND there are still moments of beauty in my life.”
“I hate my disease AND I’m grateful for the people who show up.”
“I’m grieving the life I planned AND I’m building something meaningful now.”
“This is unfair AND I’m stronger than I realized.”
This blog post is for those of us living with chronic illness who are tired of toxic positivity, but curious about what authentic gratitude practice might look like. It’s for people in pain, and for those of us holding both grief and hope.
Don’t want the science and just want the techniques? Jump ahead here.
The Science Behind Gratitude and Chronic Illness
Before we dive into practices and techniques, let’s look at why any of this matters to people who have chronic illness like RA.
In 2017, researchers studied people living with arthritis (and inflammatory bowel disease) to see if a gratitude practice affected their health1. The results showed that the people who practiced gratitude had significantly lower levels of depression. Not only this, but the gratitude practice had a bigger effect on the mental health of the chronically ill group than the healthy control group. For those of us managing chronic illness, gratitude could have major impacts.
Sleep is another area affected by gratitude practice. One study looked at how gratitude relates to sleep quality2. People who scored higher on gratitude measures fell asleep faster, slept longer, and woke up fewer times during the night. What’s happening here? The gratitude exercise helped participants replace worry with more positive thoughts. Have you ever been lying in bed, ruminating over pain or an upcoming appointment? A gratitude practice might just help you get to sleep. And sleep for us chronically ill is important – poor sleep can make pain feel worse, make fatigue worse, or even trigger a flare.
Speaking of pain, it turns out that a simple gratitude exercise could help us better cope with it3. Just like the bedtime writing exercise interrupted rumination on negative thoughts, gratitude practice at any time of day can have the same effect to refocus our thoughts on more positive things. Instead of catastrophizing, gratitude can help us reframe thoughts. Yes, I’m in pain now AND I can still do some things I value. When we practice gratitude and reframe our thoughts, we often notice the people who help us through our chronic illness struggles. Studies show that social networks can be one indicator of our ability to deal with pain3, so noticing and appreciating the people around us can also help fight pain.
In what kind of sounds like a virtuous cycle to me, some research points to better medication adherence in people who practice gratitude4. Noticing that our treatments make us feel better (even marginally) makes it easier to continue and stick with treatment plans, even through side effects and inconveniences. Appreciating our healthcare providers can help develop better, more trusting relationships with them, allowing for open communication and sticking to recommended treatments. As noted earlier, practicing gratitude can lessen depression. There is a clear link between depression and sticking with treatment, so alleviating depression usually leads to better medication adherence.
Finally, this is extremely preliminary and has not been replicated, but one small study showed that heart failure patients who kept a gratitude journal had lower inflammatory markers and overall better well-being than a control group that did not journal5. We will have to see if this study can be repeated on larger cohorts, but in the meantime if something as non-invasive as a gratitude journal could help lessen inflammation? Sign me up.
The Neuroscience: Why Does This Work?
So what’s actually happening in our brains and bodies when we practice gratitude?6
Your brain’s reward center gets LIIIIIT. When you focus on gratitude, the same neural circuits that activate during pleasure, social bonding, and stress relief go off. Your brain is literally reinforcing gratitude as a positive experience.
It interrupts the negativity loop. Our brains have a negativity bias. Perhaps you’ve noticed how easy it is to focus on medication side effects, instead of what positives the meds could do for you. We’re wired to focus on threats and problems. Gratitude practice actively disrupts this tendency. It pumps the brakes on rumination that feeds anxiety and depression. Instead of your thoughts spinning in circles about what’s wrong, gratitude gives your brain something else to consider.
It helps regulate stress. Research shows that regular gratitude practice is associated with better heart rate variability (a sign of a healthy, flexible nervous system), lower blood pressure, and an improved ability to handle stress. Your autonomic nervous system (the part that controls your fight-or-flight response) literally functions better.
It strengthens social bonds. When we express gratitude to others, it strengthens those relationships. And strong social support is one of the most powerful predictors of better health outcomes in chronic illness. There are so many options for connection in the chronic illness space. Two of my favorites are Arthritis Foundation Connect Groups and Rheum to THRIVE.
The point is, gratitude isn’t just a nice thoughts and a warm fuzzy feeling. It creates actual changes in how our brains and bodies function.
The Important Piece: Emotional Complexity
So what makes a gratitude practice different from toxic positivity? Something called emotional complexity.
Research shows that people who can experience multiple emotions simultaneously, even contradictory ones, actually have better mental health than people who try to force themselves to feel only “positive” emotions.7
The people who do best psychologically are the ones who can feel both sadness AND joy. Both grief AND gratitude. Both anger AND hope. Both frustration AND appreciation.
It’s not either/or. It’s both/and.
Gratitude practice isn’t about replacing negative emotions, it’s about making space to include positive emotions alongside the difficult ones.
When someone tells you “just be grateful” after you share your pain, they’re asking you to replace one emotion with another. That’s toxic positivity, and it’s harmful.
When you practice gratitude while also honoring your pain, anger, and grief, you’re acknowledging the full complexity of your experience as a human being with a chronic illness. You’re saying “this is hard AND there are still moments of beauty.” Both are true.
Gratitude Myths We Need to Bust
Before we get into the practical gratitude techniques, let’s clear up some harmful misconceptions…
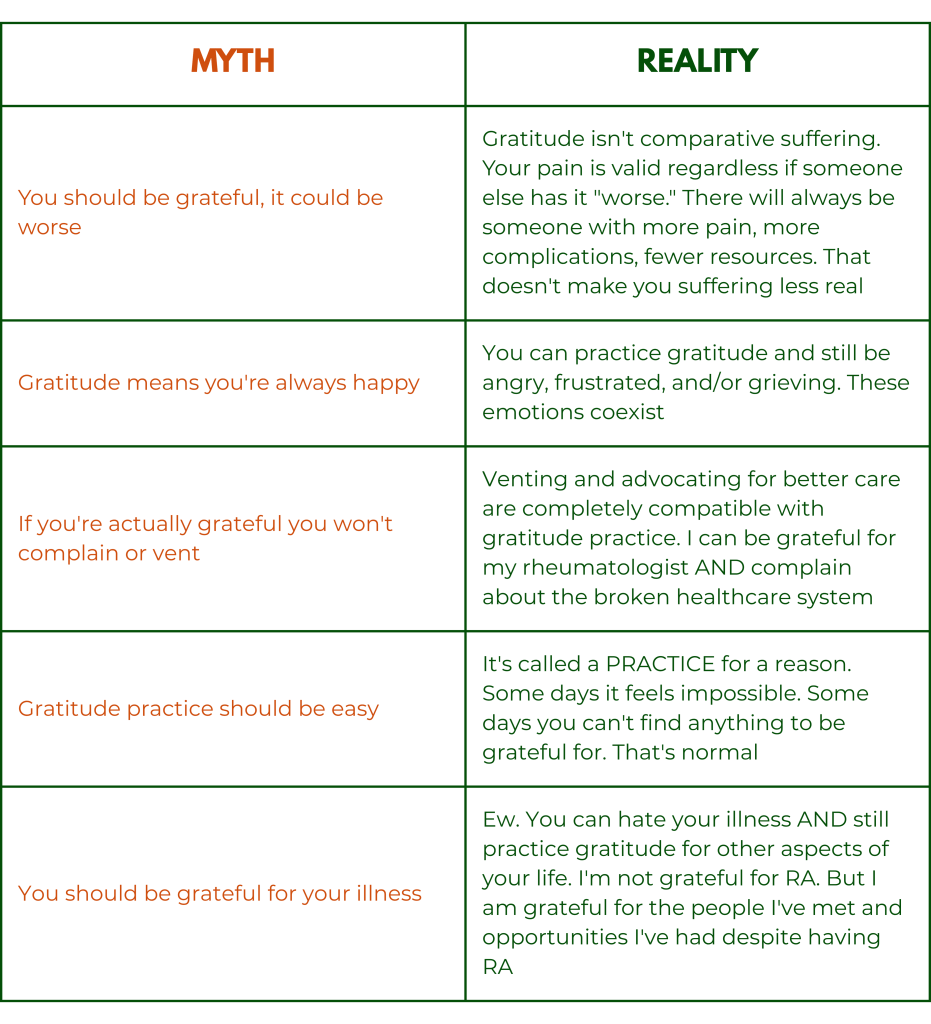
8 Gratitude Techniques Adapted for Chronic Illness
OK, time for the main event. Here are EIGHT evidence-based gratitude techniques specifically adapted for people living with chronic illness. Try one or try them all. Skip the ones that don’t land. This is about finding what works for you.
Technique 1: The “Small Good Things” Practice
What it is: Noticing tiny, specific moments rather than forcing big, abstract gratitude.
Why it works for chronic illness: When you’re in pain, big, sweeping gratitude statements feel impossible and fake. “I’m grateful for my health” might not make sense to you if you don’t feel like you have health. “I’m grateful for my RA journey” can feel dismissive when you’re suffering. But small, specific observations can feel authentic even on terrible days.
The research: Studies show that being specific matters in gratitude practice. Generic statements (“I’m grateful for my family”) are less effective than specific ones (“I’m grateful my brother texted to check on me today”).
How to do it: Each evening (or whenever works for you), notice 1-3 small, specific things from your day. Focus on sensory details and concrete moments.
Examples:
- “The heating pad felt awesome on my knees”
- “My Diet Coke was extra crispy today”
- “My friend sent me a meme that made me laugh out loud”
- “My pain was a 5 instead of an 8 today”
What this is NOT:
- “I’m grateful for my health” (can feel fake)
- “I’m grateful for my RA journey” (you don’t have to be!)
- “I’m grateful this happened to me” (no!)
- Any other big, abstract concepts that feel forced
How to start: Right now, think about the past 24 hours. What’s ONE small, specific thing you can remember? No matter how tiny or insignificant you might think it is. That’s the point.
Write it down or just notice it. That’s it. That’s the practice. Congrats, you’re practicing gratitude as a chronically ill person!!
Download the “Small Good Things” tracking sheet — part of your free starter kit
Technique 2: Gratitude Letters to Your Body Parts that Still Work
What it is: Writing short letters (mental or physical) to body parts that are still functioning.
Why it works for chronic illness: Chronic illness makes us hyper-focused on what’s broken. We worry about our painful joints, our malfunctioning immune systems, our unreliable bodies constantly. This technique redirects attention to what’s still working, without dismissing what isn’t.
The research: Research on body gratitude shows that appreciating functional body parts improves body image and increases self-compassion.
How to do it: Write a short letter to a body part that’s working for you. You can write it in a journal, type it on your phone, or just think it mentally.
Examples:
“Dear Left Knee,
I know Right Knee is down bad. I know you’re probably scared you’re next. But thank you for still bending, for still holding my weight, for still letting me walk to the bathroom in the middle of the night. You’re holding down the fort, and I see you.
Love, Me”
“Dear Eyes,
Thank you for still working (even if we need glasses — we all need some help sometimes). Thank you for letting me read, watch sunsets, see my friends’ faces, and scroll through memes when I’m sad. I don’t take you for granted.
Love, Me”
“Dear Hands,
I know mornings are rough. I know your knuckles hurt and your joints are stiff. But thank you for the afternoons when you cooperate. Thank you for still letting me type, hold my mug of tea, and hug the people I love. You’re doing great, sweetie!
Love, Me”
Important notes: This is NOT about pretending everything is fine. You can feel grateful for the things that are working, AND angry about the broken parts. Some days this feels impossible. That’s ok, skip it.
The key: You’re cultivating appreciation for things you might otherwise overlook, not ignoring pain and dysfunction.
Technique 3: The “AND” Practice (Both/And Thinking)
This one is my personal favorite.
What it is: Holding two truths simultaneously by using the word “AND” instead of “BUT.”
Why it works for chronic illness: “BUT” creates a hierarchy. It makes it seem that one truth cancels out the other. “AND” allows both truths to coexist.
The research: Studies show that “BUT” negates what comes before it, while “AND” allows for complexity (remember how important emotional complexity is?).
How to do it: Notice when you use “BUT” in your self-talk and replace it with “AND.”
Examples:
Instead of “I’m in pain, BUT I should be grateful I can still walk” (the “but” dismisses the pain), try “I’m in pain, AND I’m grateful I can still walk” (both things are true)
Instead of: “I’m struggling with fatigue, BUT at least I don’t need a wheelchair” (yikes)
Try: “I’m struggling with fatigue, AND I’m grateful for my current mobility” (yay)
Instead of: “I’m devastated about cancelling plans, BUT I should be grateful I was invited.”
Try: “I’m devastated about cancelling plans, AND I’m grateful I have friends who understand I can’t always make it.”
Instead of: “I hate my body, BUT I should love it for what it does.”
Try: “I’m angry at my body for failing me, AND I appreciate the parts that still work.”
Instead of: “This disease ruined my life, BUT others have it worse.”
Try: “This disease changed my life profoundly, AND it has provided some fun and interesting opportunities.”
The formula: [Hard truth] AND [Acknowledgment/gratitude]
Both get to be true, neither is more important. You don’t have to choose!
Practice right now: Think of something genuinely difficult about your chronic illness. Now add “AND” followed by something you can genuinely acknowledge (not something you “should” feel grateful for).
“I __________(hard truth) AND __________(acknowledgment).”
Technique 4: Gratitude for Support Systems (People, Tools, Systems)
What it is: Acknowledging the people, tools, medications, accommodations, or systems that help you survive chronic illness.
Why it works for chronic illness: It reinforces that you’re not alone. Research consistently shows that social connection is one of the strongest predictors of better health outcomes in chronic illness. Acknowledging support strengthens those connections.
How to do it: Regularly (weekly or whenever), think about or write down:
People:
- Who checked on you this week?
- Who made you laugh?
- Who believed you when you said you were in pain?
- What healthcare provider actually listened?
Tools:
- What accessibility tools make your life easier?
- What medication helps (even if it’s not perfect)?
- What app or technology supports you?
Systems:
- What online community supports you?
- What support group validates your experiences?
- What delivery service makes life easier?
Examples:
“I’m grateful for:
- My rheumatologist who takes my pain seriously (people)
- My heating pad (tools)
- My electric jar opener (tools)
- My online RA community who understands (people/systems)
- Methotrexate (even though I hate taking it, it helps) (tools)
- My compression gloves (tools)
- Voice-to-text when my hands don’t want to cooperate” (systems)
Important notes: These don’t have to be perfect. My rheumatologist isn’t perfect but I’m still grateful for them. You can be grateful for something AND frustrated by its limitations. This also isn’t about forcing gratitude for things that don’t help. And if you truly have no support, that’s valid, and something to work on addressing.
Practice right now: Express gratitude to one person this week. A simple text: “Hey, I was thinking about how much it means when you [specific thing]. Thanks!” Research shows that expressing gratitude strengthens relationships even more than feeling it privately.
Technique 5: Grief AND Gratitude Journal
What it is: A journal with two columns that honors BOTH realities of chronic illness.
Why it works for chronic illness: Sometimes gratitude practice asks us to focus only on the positive, which invalidates our very real grief and pain. This technique explicitly makes space for BOTH.
The research: Chronic illness research shows that making space for grief while ALSO cultivating positive emotions leads to better mental health outcomes.
How to do it: Create a journal (or just a piece of paper) with two columns:
| GRIEF | GRATITUDE |
|---|---|
| What I’m grieving, angry about, struggling with | What I can acknowledge or appreciate |
Examples:
| GRIEF | GRATITUDE |
|---|---|
| I miss being able to run 5Ks. | I’m grateful I can still walk my dog around the block. |
| I’m angry I need so many medications. | I’m grateful these medications exist and I have access to them. |
| I grieve my old social life and spontaneity. | I’m grateful for the friends who understand when I cancel. |
| I hate that my career plans changed. | I’m grateful I found work I can do from home. |
| I’m devastated by the financial burden of this disease. | I’m grateful for the disability benefits I was finally approved for. |
| I miss my old body. | I’m grateful for my left knee that still works. |
Important notes: The grief column is just as important as the gratitude column. Some days the grief column is longer – that’s ok. Some days you might only have grief and that’s ok, too. This isn’t about “balancing out” grief with gratitude, it’s about acknowledging that both exist.
Variation: If two columns feel too structured, just write freely, allowing both grief and gratitude to flow.
“I’m so tired today. The fatigue is overwhelming and I hate it. I had to cancel plans again and I’m grieving the social life I used to have. AND I’m grateful my friends understood without making me feel guilty. I’m grateful I have a comfortable bed to rest in. I’m grateful my heating pad exists.”
Download the Grief + Gratitude Journal template — part of your free Starter Kit
Technique 6: Sensory Gratitude Practice
What it is: Use your five senses to find moments of appreciation during pain or difficult symptoms.
Why it works for chronic illness: When pain is overwhelming, some gratitude practices feel impossible. But sensory experiences are concrete, immediate, and have the possibility to coexist with pain.
The research: Mindfulness practices (which include sensory awareness) reduce pain catastrophizing and improve quality of life in chronic pain patients.
How to do it: When you’re struggling, slowly move through each sense and find one thing to notice or appreciate:
SIGHT: What’s one thing you can see that’s pleasant?
- Sunlight through the window
- Your pet’s face
- A favorite photo
- The color of your blanket
- Flowers on your kitchen table
SOUND: What’s one sound that’s not unpleasant?
- Birds outside
- Rain on the roof
- A favorite song
- Silence (if noise is overwhelming)
SMELL: What’s one smell you appreciate right now?
- Coffee brewing
- Fresh laundry
- A candle
- Something delicious in the oven
- Clean sheets
TASTE: What’s one taste you can appreciate?
- Your favorite tea
- A piece of chocolate
- Cold Diet Coke when you’re thirsty
- Your morning medication going down (you’re taking care of yourself)
TOUCH: What’s one physical sensation that feels ok or good?
- Heating pad warmth
- A blanket’s softness
- Your cat’s purrs
- Cold water on your face
Why this works during pain: You’re not denying pain or pretending it doesn’t exist. You’re simply noticing that pain isn’t the ONLY sensation present. Other sensory experiences coexist with pain.
This is a mini mindfulness practice that grounds you in the present moment and reduces rumination. I’ve used this technique when experiencing a migraine but didn’t have medication with me and couldn’t access any. Mindfulness didn’t cure the migraine, but using this sensory practice allowed me to focus on other things besides JUST the pain.
Example:
“I’m in a terrible flare right now. My pain is an 8/10. AND I can also feel the warmth of my heating pad, hear my dog snoring, smell the lavender from my diffuser, see the sunset through my window, and taste my peppermint tea. The pain is real. These things are also real.”
Technique 7: Gratitude for Your Resilience
What it is: Acknowledging the incredible strength it takes to live with chronic illness.
Why it works for chronic illness: We rarely give ourselves credit for what we endure daily. Research shows that self-compassion and acknowledging our own resilience reduces depression and improves coping.
How to do it: Regularly (maybe once a week), acknowledge what you’ve survived and how hard you’re working.
Prompts:
- What did you accomplish this week despite your illness?
- What symptom did you manage well?
- What appointment did you advocate for yourself in?
- What challenge did you face that healthy people don’t even think about?
- What adaptation did you create?
- What bad day did you survive?
Examples:
“I’m grateful for my own resilience. I made it through a week-long flare. I advocated for myself when my doctor dismissed my pain. I figured out a workaround when my hands wouldn’t cooperate. I asked for help even though it’s hard. I took my medications even when I didn’t want to. I rested without guilt (or tried to!). I showed up for myself when no one else could.”
Or, try writing a letter to yourself:
“Dear Me,
You are doing an incredibly hard thing. You wake up every day in a body that’s fighting itself. You manage medications, appointments, pain, fatigue, and unpredictability. You’ve had to grieve the life you planned and build something new. You keep going even when it’s excruciating.
That’s not nothing, that’s heroic. I’m grateful for your strength.
Love, Me”
Technique 8: Future Gratitude Visualization
What it is: Imagining future moments you’ll be grateful for, which creates hope alongside current suffering.
Why it works for chronic illness: Research on “prospective gratitude” (anticipating future good things) shows it increases hope and reduces depression. When you’re in a flare, remembering that it is temporary can help.
How to do it: When you’re struggling, imagine a specific moment in the near future that you’ll appreciate.
Examples:
“Right now I’m in terrible pain. But in a few days, this flare will calm down, and I’ll be grateful for that relief. I’ll appreciate being able to take a walk without my knees screaming. I’ll be grateful to sleep through the night. I’m not there yet, but I will be.”
“This medication change has me crashing out right now. But in a few weeks, if it works, I’ll be grateful for reduced inflammation. I’ll be grateful for mornings with less stiffness. I’m holding onto that possibility.”
Why this works:
- It acknowledges that your current state isn’t permanent
- It creates something to hold onto during dark times
- It reminds you that relief has come before and will come again
- It’s not toxic positivity (you’re not pretending that you feel good right now)
Important: This isn’t about “silver linings” or “everything happens for a reason.” It’s about knowing that chronic illness has downs…and it also has ups. Flares end, bad days pass, medications sometimes work. It sounds cliché, but it’s true: you’ve survived 100% of your worst days so far.
When Gratitude Practice Feels Impossible
Let’s talk about when gratitude practice just doesn’t work, feels fake, or makes you feel WORSE.
This is completely normal and valid.
When to SKIP gratitude practice:
- During acute crisis
- Severe flare-ups
- Hospitalization
- Medical emergencies
- Recent traumatic diagnosis
> Right now, survival is the priority. Gratitude can wait.
- When you’re in deep grief
- Processing a major loss related to your illness
- Coming to terms with new limitations
- Grieving who you were before diagnosis
> Grief needs space and time. Forcing gratitude during grief is harmful.
- When it triggers toxic positivity trauma
- If gratitude practice reminds you of people who dismissed your pain
- If it makes you feel like you’re not allowed to be sad
> Your mental health matters more than any practice.
- When you’re exhausted
- Severe fatigue
- Brain fog
- Barely functioning
> Rest is more important. You don’t need to earn rest with gratitude.
What to do instead: When gratitude practice isn’t working, try:
- Just acknowledging reality: “This is hard. I’m in pain. This sucks. That’s the truth right now.”
- Rage journaling: Write out every angry, bitter, unfair thought without trying to find gratitude. Sometimes you need to purge the bad feelings before you can access anything else.
- Seek support: Talk to someone who gets it. Call your therapist. Post in your online community. Sometimes we need validation, not gratitude.
- Give yourself permission: “I don’t have to practice gratitude today. I’m allowed to just feel terrible.” When I’m having a particularly bad flare or difficult mental health day I give myself 1 day to just wallow in feeling terrible.
When gratitude practice brings up difficult emotions: Sometimes gratitude practice makes you feel worse temporarily. This can happen when it highlights what you’ve lost, makes you realize how much you’ve been suppressing, or brings up grief you haven’t processed.
This isn’t a sign you’re doing it wrong. Sometimes acknowledging goodness makes you aware of how much bad you’ve been enduring. If this happens:
- Stop the practice. You don’t have to continue.
- Let yourself feel the feelings. Cry, journal, talk it out.
- Reach out for support if needed.
- Consider therapy . If this keeps happening it might indicate unprocessed trauma or grief.
Signs gratitude practice is becoming toxic. Stop and reassess if you notice:
- You feel guilty when you’re not grateful.
- You’re using gratitude to avoid negative emotions.
- You’re dismissing your own pain with “at least” statements.
- You feel like you have to earn complaining by first listing gratitude.
- Other people use your gratitude practice to dismiss your struggles.
- You feel worse about yourself when you can’t find gratitude.
Healthy gratitude practice should expand your emotional range, not reduce it.
Ready to Try a Gratitude Practice?
I’ve created a completely free starter kit with everything you need to begin your own gratitude practice.
What’s included:
- The “Small Good Things” Tracking Sheet
- 30-day tracker for noticing daily moments
- Grief + Gratitude Journal Template
- Two-column format
- Weekly and daily versions
- “AND” Practice Worksheet
- Fill-in prompts to practice Both/And thinking
- Body Gratitude Letter Templates
- Starter prompts for writing to your body parts
- Sensory Gratitude Checklist
- All 5 senses with prompts
- Quick Reference Guide
- All 8 techniques summarized on 1 page
- Print and keep by your bed
- Gratitude Myths Debunked
- Printable reminder of what gratitude is NOT
- Share with people who don’t understand
CLICK HERE TO DOWNLOAD YOUR FREE GRATITUDE STARTER KIT
No email required, you’re already dealing with enough. Just download and use.
References
- Sirois, F. M., & Wood, A. M. (2017). Gratitude uniquely predicts lower depression in chronic illness populations: A longitudinal study of inflammatory bowel disease and arthritis. Health Psychology, 36(2), 122-132. https://doi.org/10.1037/hea0000436
- Wood, A. M., Joseph, S., Lloyd, J., & Atkins, S. (2009). Gratitude influences sleep through the mechanism of pre-sleep cognitions. Journal of Psychosomatic Research, 66(1), 43-48. https://doi.org/10.1016/j.jpsychores.2008.04.002
- Ng, M. Y., & Wong, W. S. (2013). The differential effects of gratitude and sleep on psychological distress in patients with chronic pain. Journal of Health Psychology, 18(2), 263-271. https://doi.org/10.1177/1359105311433906
- Boggiss, A. L., Consedine, N. S., Brenton-Peters, J. M., Hofman, P. L., & Serlachius, A. S. (2020). A systematic review of gratitude interventions: Effects on physical health and health behaviors. Journal of Psychosomatic Research, 135, 110165. https://doi.org/10.1016/j.jpsychores.2020.110165
- Redwine, L. S., Henry, B. L., Pung, M. A., Wilson, K., Chinh, K., Knight, B., … & Mills, P. J. (2016). Pilot randomized study of a gratitude journaling intervention on heart rate variability and inflammatory biomarkers in patients with stage B heart failure. Psychosomatic Medicine, 78(6), 667-676. https://doi.org/10.1097/PSY.0000000000000316
- Fox, G. R., Kaplan, J., Damasio, H., & Damasio, A. (2015). Neural correlates of gratitude. Frontiers in Psychology, 6, 1491. https://doi.org/10.3389/fpsyg.2015.01491; Redwine et al., 2016 (cited above); Wood et al., 2009 (cited above); various studies on social support and health outcomes in chronic illness populations
- Rafaeli, E., Rogers, G. M., & Revelle, W. (2007). Affective synchrony: Individual differences in mixed emotions. Personality and Social Psychology Bulletin, 33(7), 915-932. https://doi.org/10.1177/0146167207301009






Leave a comment